Dilation and Curettage (D&C): A Comprehensive Overview
Dilation and curettage (D&C) effectively removes uterine contents via cervical dilation and scraping.
Downloadable guides offer detailed insights into the process, recovery, and expectations, providing crucial patient education.
What is Dilation and Curettage (D&C)?
Dilation and curettage (D&C) is a gynecological procedure involving the widening, or dilation, of the cervix. This allows access to the uterine cavity for the removal of tissue, achieved through a surgical scraping of the uterine lining – a process called curettage. It’s a versatile procedure utilized for both diagnostic and therapeutic purposes.
Essentially, a D&C involves gently opening the cervical canal and then employing a specialized instrument, the curette, to carefully remove tissue from the uterus. Comprehensive guides, often available as downloadable PDFs, detail this process. These resources explain how the procedure works, emphasizing the careful technique needed to avoid complications. The procedure is performed to obtain uterine tissue samples or to clear the uterine cavity of contents.
Understanding the specifics of D&C, as outlined in detailed procedure guides, empowers patients with knowledge about their healthcare journey.
Purpose of a D&C Procedure
The dilation and curettage (D&C) procedure serves multiple crucial purposes in women’s healthcare. Primarily, it’s employed to diagnose and treat abnormal uterine bleeding, offering a pathway to identify underlying causes. Detailed PDF guides highlight this diagnostic role, explaining how tissue samples are analyzed.
Furthermore, a D&C is frequently used to manage complications related to pregnancy, specifically first-trimester pregnancy failure. It effectively removes incomplete miscarriage tissue, preventing infection and aiding physical recovery. These guides also emphasize its use in managing early pregnancy loss.
Beyond these core applications, a D&C can remove retained placental tissue after childbirth. Comprehensive resources detail the procedure’s versatility, emphasizing its importance in both diagnostic evaluations and therapeutic interventions. Understanding these purposes, as outlined in downloadable materials, is vital for informed patient care.
Indications for D&C: First Trimester Pregnancy Failure
A dilation and curettage (D&C) is a common intervention for first-trimester pregnancy failure, encompassing miscarriage, incomplete abortion, or blighted ovum. PDF resources detail these scenarios, explaining how a D&C effectively removes retained tissue, minimizing risks of infection and hemorrhage.
Clinically significant blood loss is a key consideration; identifying patients at risk informs the decision regarding the procedure’s setting – inpatient versus outpatient. Guides emphasize careful patient assessment to determine the appropriate approach.
The procedure addresses incomplete passage of pregnancy tissue, preventing prolonged bleeding and potential complications. Comprehensive D&C information resources highlight the importance of timely intervention in these cases; Downloadable guides provide detailed explanations of the indications, ensuring patients understand the necessity of the procedure for their health and well-being.
D&C for Abnormal Uterine Bleeding
Dilation and curettage (D&C) serves as both a diagnostic and therapeutic tool for abnormal uterine bleeding (AUB). PDF guides explain how a D&C can help identify the cause of irregular or heavy bleeding by providing tissue samples for pathological examination.
The procedure can directly address AUB by removing thickened endometrial lining or polyps, reducing bleeding and restoring normal menstrual cycles. Comprehensive resources detail how a D&C can be utilized when hormonal imbalances or structural abnormalities are suspected.
Detailed D&C procedure guides emphasize that the procedure is often included in episodes for diagnosis or treatment of AUB. Downloadable materials clarify the process, recovery, and potential risks, empowering patients with knowledge about their care and treatment options for managing abnormal uterine bleeding.
D&C as a Diagnostic Tool
Dilation and curettage (D&C) is a valuable diagnostic procedure, enabling the examination of uterine tissue to identify the cause of various gynecological issues. Downloadable PDF resources highlight how a D&C allows for the collection of endometrial samples for pathological analysis, crucial for accurate diagnosis.
These guides explain that a D&C can help detect abnormalities like endometrial hyperplasia, polyps, or even uterine cancer. The procedure is frequently utilized in cases of abnormal uterine bleeding or to investigate the cause of infertility.
Comprehensive D&C information resources detail how the collected tissue is sent to a laboratory for microscopic evaluation, providing vital information for treatment planning. Patient guides emphasize the importance of understanding the diagnostic role of a D&C and the subsequent steps in their care.
Preparing for Your D&C Procedure
Patient guides detail pre-procedure instructions, including avoiding drugs like aspirin. Thorough preparation, outlined in downloadable PDFs, ensures a smoother experience and optimal outcomes.
Pre-Procedure Instructions: Medications to Avoid
Prior to your D&C procedure, carefully review medication guidelines provided in comprehensive patient resources, often available as downloadable PDFs. It’s crucial to inform your healthcare provider about all medications you are currently taking, including over-the-counter drugs and herbal supplements.
Specifically, avoid medications that can increase bleeding risk. This includes aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve), and other nonsteroidal anti-inflammatory drugs (NSAIDs) – typically for at least one week before the procedure. Your doctor may also advise you to stop taking blood thinners, such as warfarin (Coumadin) or clopidogrel (Plavix), several days beforehand, depending on your individual health status.
Discuss any necessary adjustments to your medication regimen with your physician. Failure to adhere to these instructions could potentially lead to increased bleeding during or after the D&C. Detailed PDF guides often contain a complete list of medications to avoid and specific timelines for discontinuation.
Pre-Procedure Examination: Bimanual and Rectovaginal Exam
A thorough pelvic examination is a vital component of pre-D&C preparation, detailed in many downloadable procedure guides. This includes both a bimanual exam – where the healthcare provider inserts gloved hands into the vagina and abdomen to assess the uterus’ size, position, and tenderness – and a rectovaginal exam.
The rectovaginal exam involves simultaneously inserting a hand into the vagina and a gloved finger into the rectum. This allows the provider to evaluate the uterosacral ligaments and the posterior aspect of the uterus, helping to identify any abnormalities or potential challenges during the D&C.
These examinations help determine uterine size and position, assess for any pelvic masses, and evaluate the cervix. This comprehensive assessment is crucial for safe and effective procedure planning, minimizing risks like uterine perforation, as outlined in comprehensive D&C resources.
Fasting Requirements Before a D&C
Strict adherence to fasting guidelines is paramount before undergoing a Dilation and Curettage (D&C) procedure, as detailed in patient instruction PDFs. Typically, patients are instructed to refrain from eating or drinking anything – including water – for a specific period, usually six to eight hours, prior to the scheduled procedure time.
This fasting requirement is crucial because a D&C often involves the administration of anesthesia, whether local, sedation, or general anesthesia. Having food or liquids in the stomach can significantly increase the risk of complications such as nausea, vomiting, and, more seriously, aspiration during anesthesia.
Detailed D&C procedure guides emphasize the importance of clarifying these fasting instructions with your healthcare provider and diligently following their specific recommendations to ensure a safe and smooth surgical experience.
Informed Consent and Patient History
Comprehensive informed consent is a cornerstone of the D&C process, thoroughly outlined in downloadable procedure PDFs. Before proceeding, patients must receive detailed information about the reasons for the D&C, the procedure itself, potential risks and benefits, and alternative treatment options.
A meticulous review of the patient’s medical history is equally vital. This includes documenting any existing medical conditions, allergies (especially to medications or latex), current medications (specifically noting aspirin or blood thinners which may need adjustment), and previous surgical procedures.
Detailed D&C information resources stress the importance of honest and open communication with your healthcare provider, ensuring you fully understand the procedure and have the opportunity to address any concerns or questions before signing the consent form.
The D&C Procedure: What to Expect
During a D&C, the cervix dilates, and a curette removes uterine tissue. Detailed PDFs illustrate patient positioning and techniques to minimize uterine perforation risks.
Patient Positioning During D&C
Optimal patient positioning is crucial for a safe and effective Dilation and Curettage (D&C) procedure. Typically, the patient is placed in the dorsal lithotomy position, which involves lying on their back with their legs raised and supported in stirrups.
This positioning provides excellent access to the cervix and uterus for the surgeon. The legs are carefully placed in appropriate gynecologic stirrups, ensuring stability and comfort for the patient throughout the procedure. Proper positioning facilitates optimal visualization and manipulation of instruments within the uterine cavity.
Comprehensive D&C procedure guides, often available as downloadable PDFs, frequently include detailed illustrations of the correct patient positioning. These resources emphasize the importance of ensuring the patient is securely and comfortably positioned before the procedure begins, contributing to both patient safety and surgical success. Careful attention to positioning minimizes potential complications and enhances the overall procedural outcome.
Cervical Dilation Techniques
Cervical dilation is a critical step in Dilation and Curettage (D&C), enabling access to the uterine cavity. Several techniques are employed, ranging from mechanical dilation using progressively larger dilators to pharmacological methods utilizing medications like misoprostol to soften and open the cervix.
Care must be taken during dilation to avoid perforation of the uterus, a potential complication. Experienced surgeons carefully assess the cervix and select the most appropriate dilation method based on individual patient factors. Downloadable D&C procedure guides often detail these techniques, including step-by-step instructions and visual aids.
The choice of technique depends on factors like gestational age, cervical firmness, and patient history. Gradual dilation is generally preferred to minimize discomfort and reduce the risk of cervical injury. Proper technique is paramount for a safe and successful D&C procedure;
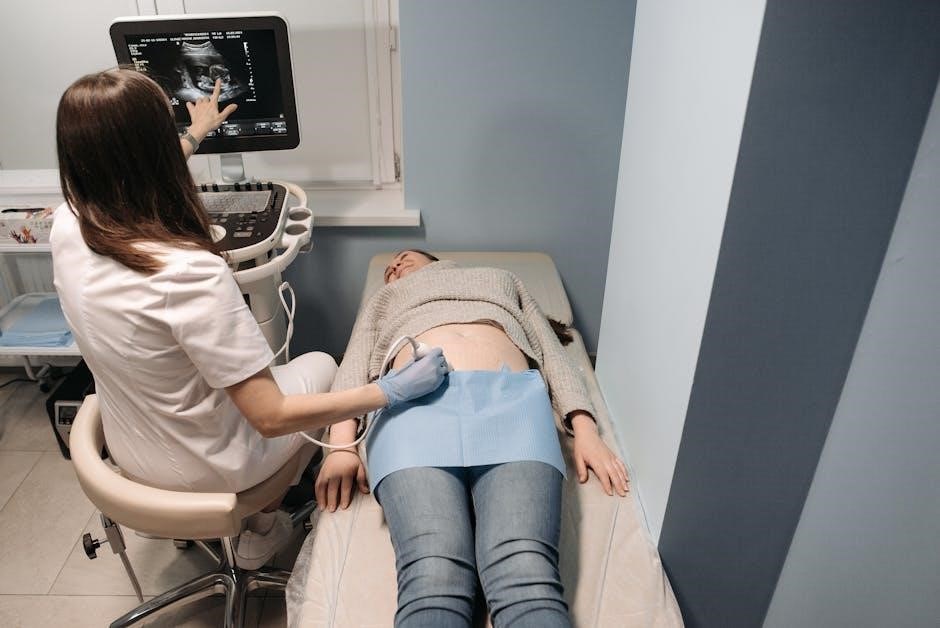
Uterine Lining Removal with a Curette
Following cervical dilation, a curette – a specialized surgical instrument – is used to gently remove tissue from the uterine lining. This process is central to a Dilation and Curettage (D&C) procedure, whether performed for diagnostic purposes or to manage pregnancy loss or abnormal bleeding.
The curette’s design allows for controlled scraping of the uterine walls, ensuring complete removal of the targeted tissue. Detailed D&C procedure guides, available for download, often illustrate the proper curettage technique, emphasizing gentle and systematic movements to minimize trauma.
Surgeons employ careful technique to avoid uterine perforation, a potential risk during curettage. Visual inspection and tactile feedback are crucial throughout the process. The removed tissue is then sent to pathology for examination, aiding in diagnosis and guiding further treatment decisions.
Minimizing Risks: Avoiding Uterine Perforation
Uterine perforation, a rare but serious complication of D&C, occurs when the curette penetrates the uterine wall. Comprehensive D&C procedure guides emphasize meticulous technique to minimize this risk. Careful cervical dilation is paramount, avoiding excessive force that could lead to uterine damage.
A thorough bimanual examination, including a rectovaginal exam, prior to the procedure helps assess uterine position and identify potential anatomical variations. Surgeons utilize gentle, controlled movements during curettage, constantly monitoring resistance and avoiding excessive depth.
Visual guidance, such as ultrasound, can further enhance safety. Should perforation occur, prompt recognition and management are crucial, potentially requiring surgical intervention. Detailed PDF resources outline the signs of perforation and appropriate response protocols for healthcare providers.
Post-Procedure Care and Recovery
Post-D&C care involves monitoring, pain management, and observing for bleeding or infection. Comprehensive guides detail recovery expectations and when to seek medical attention promptly.
Immediate Post-Operative Monitoring
Following a D&C procedure, careful monitoring is essential during the initial recovery phase. Patients are typically observed in a recovery area for one to several hours, allowing healthcare professionals to assess their vital signs – including blood pressure, pulse, and respiration – for stability.
A key focus is monitoring for excessive bleeding, which can be a sign of complications. Nurses will regularly check the uterine fundus (the top of the uterus) to ensure it feels firm, indicating effective contraction and minimizing blood loss. The amount of vaginal discharge is also closely observed.
Pain levels are assessed and managed with appropriate pain medication. Patients are encouraged to report any unusual symptoms, such as severe cramping, heavy bleeding, fever, or signs of infection. Downloadable post-operative guides often provide a checklist of symptoms to watch for and instructions on when to contact a healthcare provider. This immediate monitoring period is crucial for identifying and addressing any potential issues promptly, ensuring a smooth and safe recovery.
Managing Pain After a D&C
Post-D&C pain is common and typically managed effectively with over-the-counter or prescription pain medication. Mild discomfort, resembling menstrual cramps, is often experienced initially. Healthcare providers commonly recommend nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen to reduce pain and inflammation.
For more significant pain, a stronger prescription pain reliever may be prescribed, but should be used as directed and for a limited duration. Applying a heating pad to the lower abdomen can also provide soothing relief.
Downloadable D&C guides frequently detail pain management strategies, including recommended dosages and potential side effects of medications. It’s important to communicate with your healthcare provider about your pain levels and any concerns. Adequate pain control is crucial for a comfortable recovery, allowing patients to gradually resume normal activities.
Bleeding and Discharge After D&C
Post-D&C bleeding is expected, ranging from spotting to a light menstrual flow. Initially, heavier bleeding is possible, gradually decreasing over several days or weeks. Downloadable D&C procedure guides emphasize monitoring the amount and type of bleeding. Soaking a pad within an hour is considered heavy bleeding and requires immediate medical attention.
A brownish or pinkish discharge is common as healing progresses. Avoid using tampons, douching, or having sexual intercourse for the recommended period (usually 2-6 weeks) to prevent infection and allow the uterine lining to heal.
Comprehensive resources detail what constitutes normal versus concerning bleeding patterns. Contact your healthcare provider if you experience heavy bleeding, fever, severe pain, or foul-smelling discharge, as these could indicate complications.
Resuming Normal Activities
Gradual resumption of normal activities is key following a D&C. Downloadable D&C guides recommend resting for several days immediately post-procedure. Light activities, like walking, can be resumed when feeling comfortable, typically within a few days.
Avoid strenuous activities, heavy lifting (over 10 pounds), and vigorous exercise for at least two weeks, or as directed by your healthcare provider. These restrictions minimize the risk of complications and allow for proper uterine healing.
Sexual intercourse should be avoided for the timeframe specified by your doctor, usually 2-6 weeks, to prevent infection. Comprehensive resources emphasize listening to your body and increasing activity levels gradually, avoiding any activity that causes pain or increased bleeding.

Potential Risks and Complications of D&C
Potential risks include infection, uterine perforation, heavy bleeding, and Asherman’s Syndrome—scar tissue formation. Detailed PDF guides outline management strategies for each complication.
Risk of Infection Following D&C
Post-D&C infection, though uncommon, represents a significant concern requiring prompt attention. The introduction of instruments into the uterus inherently carries a risk of bacterial introduction, potentially leading to endometritis—inflammation of the uterine lining—or, less frequently, pelvic inflammatory disease (PID). Comprehensive D&C procedure guides, often available as downloadable PDFs, emphasize meticulous sterile technique during the procedure as a primary preventative measure.
Patients should be vigilant for signs of infection following a D&C, including fever, chills, worsening pelvic pain, foul-smelling vaginal discharge, and general malaise. Early recognition and treatment with antibiotics are crucial to prevent complications. PDF resources often detail specific antibiotic regimens commonly employed. Prophylactic antibiotics are not routinely administered, but may be considered in cases with heightened risk factors. Thorough patient education, detailed in downloadable guides, empowers individuals to recognize and report potential issues promptly, ensuring optimal outcomes and minimizing the risk of long-term sequelae.
Uterine Perforation: Causes and Management
Uterine perforation, a rare but serious complication of D&C, occurs when the instruments penetrate the uterine wall. Causes include inadequate uterine assessment prior to dilation, excessive force during dilation or curettage, and anatomical factors like a retroverted uterus. Downloadable D&C procedure guides frequently highlight the importance of a thorough bimanual and rectovaginal examination to assess uterine position and depth before commencing the procedure.
Careful and controlled dilation techniques are paramount to minimizing this risk. Management depends on the severity of the perforation; small perforations may be managed conservatively with observation, while larger perforations may require surgical repair, potentially via laparoscopy. PDF resources emphasize the need for immediate recognition – symptoms can include sudden severe pain, bleeding, or signs of internal injury. Prompt diagnosis and appropriate intervention are crucial to prevent further complications and ensure patient safety.
Heavy Bleeding and Hemorrhage
Heavy bleeding and hemorrhage represent significant risks associated with D&C procedures. Identifying patients predisposed to substantial blood loss is crucial, potentially influencing the decision regarding the appropriate setting – inpatient versus outpatient – for the procedure. Comprehensive D&C information resources, often available as downloadable PDFs, detail strategies for minimizing blood loss during the operation.
These strategies include meticulous hemostasis techniques and careful curettage to avoid excessive trauma to the uterine lining. Post-procedure, monitoring for signs of excessive bleeding is vital. Management of hemorrhage may involve uterine massage, medications to contract the uterus, or, in severe cases, blood transfusion. PDF guides emphasize the importance of reporting any unusually heavy bleeding to a healthcare provider immediately for prompt evaluation and intervention, ensuring patient stability and well-being.
Asherman’s Syndrome: Scar Tissue Formation
Asherman’s Syndrome, a rare but serious complication of D&C, involves the formation of scar tissue within the uterine cavity. Downloadable D&C procedure guides (PDF) often highlight this risk, emphasizing the importance of gentle curettage techniques to minimize uterine trauma. Excessive or aggressive curettage increases the likelihood of scar tissue development, potentially leading to menstrual irregularities, infertility, and recurrent pregnancy loss.

Diagnosis typically requires hysteroscopy to visualize the uterine cavity and identify adhesions. Treatment options, detailed in comprehensive resources, may include hysteroscopic adhesiolysis – a procedure to surgically remove the scar tissue. Patient education materials stress the importance of discussing the potential risk of Asherman’s Syndrome with their healthcare provider and reporting any subsequent menstrual changes or difficulty conceiving.
Resources and Further Information
Comprehensive D&C information is readily available through downloadable PDF guides. These resources detail the procedure, recovery, and potential risks for informed patient understanding.
Downloadable D&C Procedure Guides (PDF)
Accessing comprehensive D&C guides in PDF format empowers patients with detailed knowledge before and after the procedure. These resources typically cover all aspects, from pre-procedure preparation – including vital medication avoidance instructions like aspirin – to post-operative care expectations.
You’ll find information regarding patient positioning during the D&C, commonly the dorsal lithotomy position, and explanations of cervical dilation techniques. Guides also detail the uterine lining removal process using a curette, emphasizing the importance of minimizing risks such as uterine perforation through careful technique.
Furthermore, these PDFs often include sections on managing post-operative pain, understanding expected bleeding and discharge, and guidelines for resuming normal activities. They serve as valuable tools for informed consent and a smoother recovery journey, offering peace of mind and clarity throughout the entire process.
Comprehensive D&C Information Resources
Beyond downloadable PDFs, a wealth of online resources provides in-depth information about dilation and curettage (D&C). These resources clarify the procedure’s uses – from managing first-trimester pregnancy failure and abnormal uterine bleeding to serving as a crucial diagnostic tool.
Patients can access details about pre-procedure examinations, including the importance of a thorough bimanual and rectovaginal exam to assess uterine health. Information regarding fasting requirements before a D&C is readily available, alongside explanations of informed consent and the necessity of a complete patient history.
These resources also address potential risks and complications, such as infection, uterine perforation, heavy bleeding, and the rare occurrence of Asherman’s Syndrome. Understanding these possibilities allows for proactive discussion with healthcare providers and informed decision-making, ultimately leading to better patient outcomes and reduced anxiety.